
If it is warmed rapidly, large amounts of carbon dioxide are generated, which can be dangerous, particularly within confined areas. Solid carbon dioxide may cause burns following direct contact. Concentrations >10% may cause convulsions, coma and death. At higher concentrations it leads to an increased respiratory rate, tachycardia, cardiac arrhythmias and impaired consciousness. At low concentrations, gaseous carbon dioxide appears to have little toxicological effect. Its main mode of action is as an asphyxiant, although it also exerts toxic effects at cellular level. It is widely used in the food industry in the carbonation of beverages, in fire extinguishers as an 'inerting' agent and in the chemical industry. doi:10.1136/bmjopen-2015-008909.Carbon dioxide is a physiologically important gas, produced by the body as a result of cellular metabolism. Is hypercapnia associated with poor prognosis in chronic obstructive pulmonary disease? A long-term follow-up cohort study. Yang H, Xiang P, Zhang E, Guo W, Shi Y, Zhang S, et al. 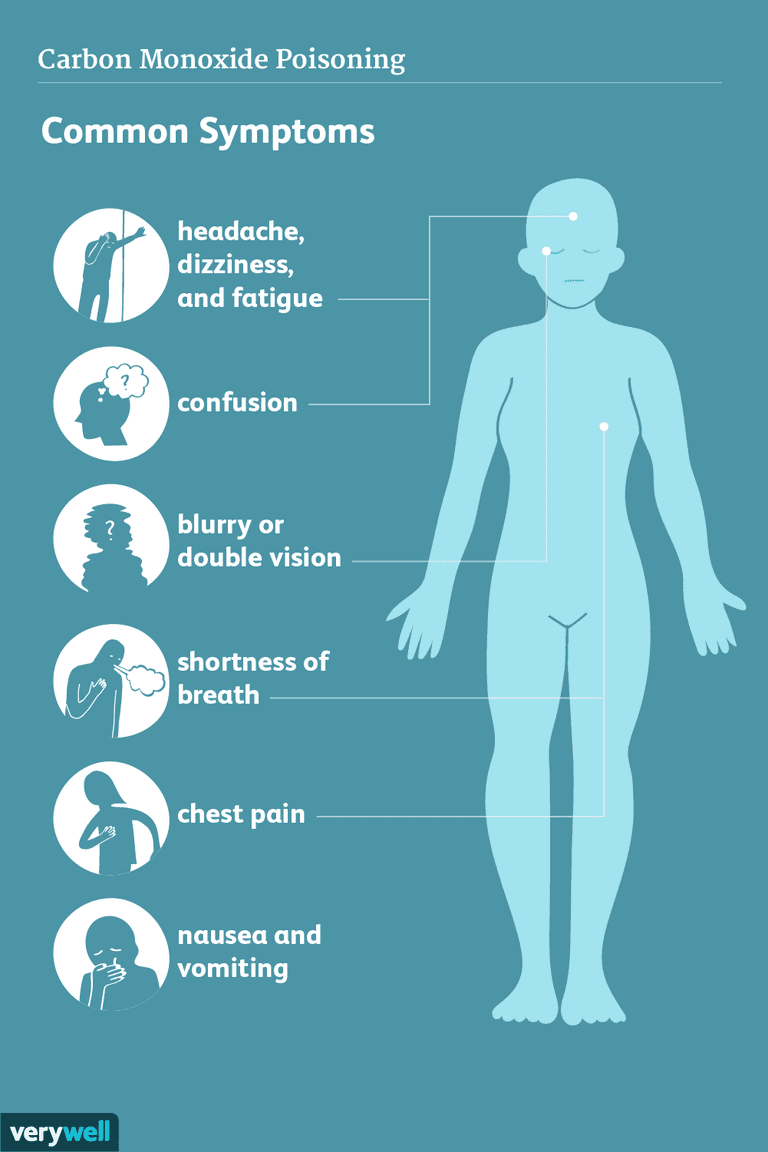
Intensive Care Med Exp. 2019 Jul 25 7(Suppl 1):39. The role of hypercapnia in acute respiratory failure. Morales-Quinteros L, Camprubí-Rimblas M, Bringué J, Bos LD, Schultz MJ, Artigas A. Hypercapnia-induced cerebral hyperperfusion: an underrecognized clinical entity. Pollock JM, Deibler AR, Whitlow CT, et al. High-flow nasal cannula versus conventional oxygen therapy in acute COPD exacerbation with mild hypercapnia: a multicenter randomized controlled trial. Xia J, Gu S, Lei W, Zhang J, Wei H, Liu C, et al. Face mask and hypercapnia in patients with COPD in COVID-19 pandemic…is it real? Chest. Carbon dioxide increases with face masks but remains below short-term NIOSH limits. Rhee MSM, Lindquist CD, Silvestrini MT, Chan AC, Ong JJY, Sharma VK. National Heart, Lung, and Blood Institute. Dyspnea in amyotrophic lateral sclerosis: the Dyspnea-ALS-Scale (DALS-15) essentially contributes to the diagnosis of respiratory impairment. Risk factors of chronic obstructive pulmonary disease exacerbations. Hogea SP, Tudorache E, Fildan AP, Fira-Mladinescu O, Marc M, Oancea C. Comorbidities and subgroups of patients surviving severe acute hypercapnic respiratory failure in the intensive care unit. 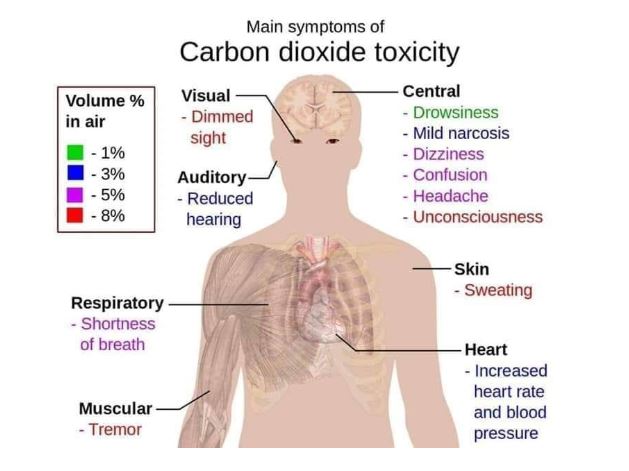
StatPearls.Īdler D, Pépin JL, Dupuis-Lozeron E, et al. Patel S, Miao JH, Yetiskul E, Anokhin A, Majmundar SH. Caffeine Use in the Anesthetic Management of a Patient With Congenital Central Hypoventilation. How the lungs work.ĭavis JS, Allais L, Abdallah C. National Heart, Lung and Blood Institute. It can vary greatly from one patient to another but can include a mix of breathing exercises, physical exercises, and diet and nutrition consultations. Pulmonary rehab is another treatment option.You must wear a device that resembles an over-the-shoulder purse or backpack with a tube (cannula) that delivers oxygen into your nose. Oxygen therapy gives you freedom of movement while you're being treated for hypercapnia.The mask is connected to a machine that delivers gentle air pressure and oxygen from a flow generator, though you can still breathe on your own. A tightly fitted mask is placed over your face or nose. Noninvasive ventilation provides breathing support through the upper airways.Mechanical ventilation involves the use of a mechanical ventilator that takes over the act of breathing for you.You may need this type of respiratory assistance temporarily while a severe medical illness is being treated. You are unable to breathe or speak while you are intubated. Intubation requires that an endotracheal tube be placed in your mouth and down into your airway.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
